What is Deep Vein Thrombosis?
DVT typically develops when blood flow slows down or changes, allowing a clot to form inside a vein. Veins have one-way valves to keep blood moving toward the heart; when a clot forms, it can damage these valves or completely block the flow of blood.
Clots are generally classified by their location:
-
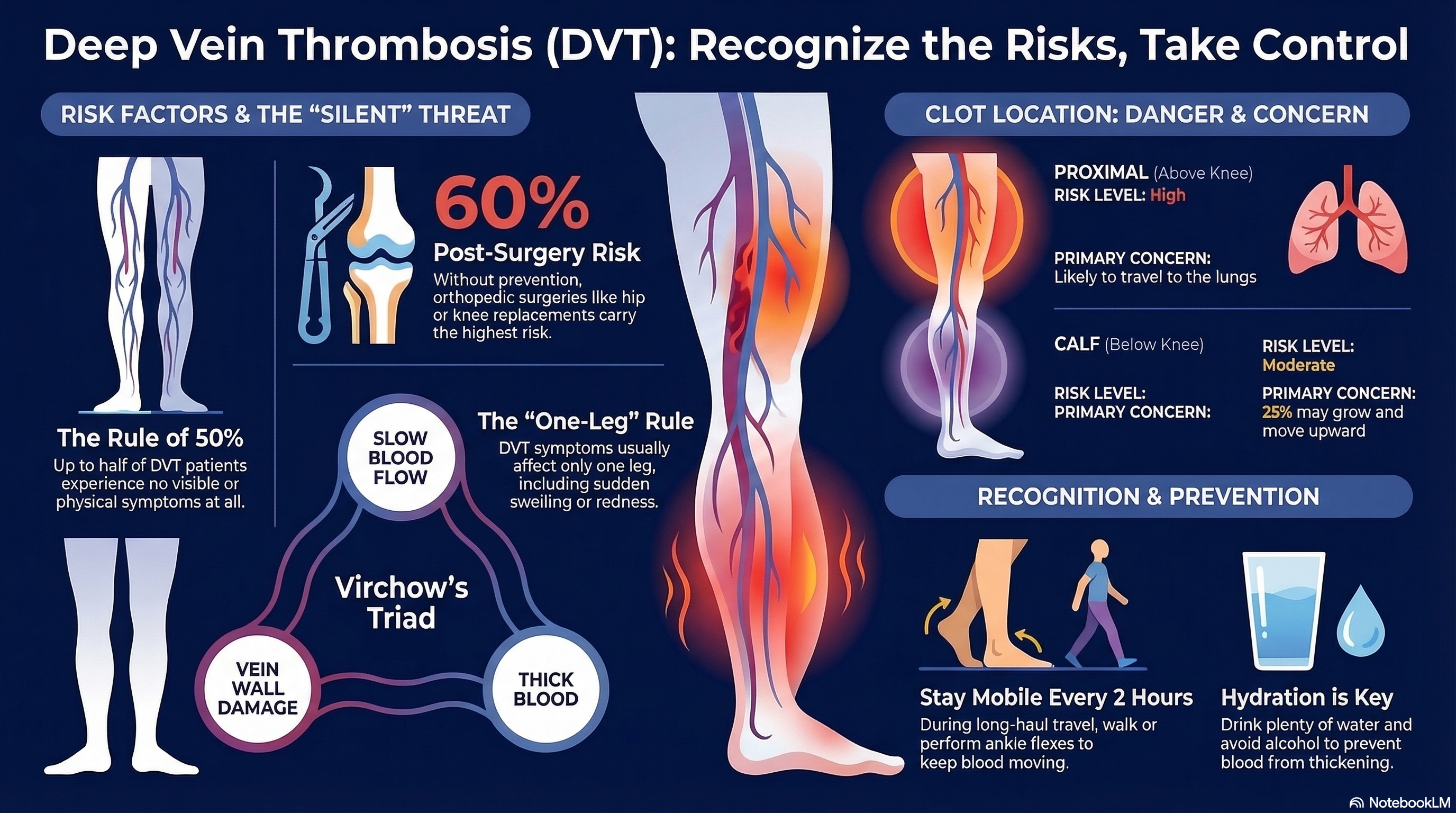
Proximal DVT: Clots located in the larger veins above the knee (popliteal, femoral, or iliac veins). These are the most dangerous as they are more likely to break off and travel to the lungs.
-
Calf DVT: Clots in the smaller veins of the lower leg. While less likely to cause a PE, about 25% of these clots can grow and move into the proximal veins if left untreated.
Causes of Deep Vein Thrombosis
Most cases of DVT result from a combination of factors known as Virchow’s Triad: slow blood flow (stasis), damage to the vein wall, and changes in the blood that make it "thicker" or more likely to clot (hypercoagulability).
Major Risk Factors:
-
Surgery and Injury: Major operations (especially hip or knee replacements) and bone fractures are significant triggers. Without prevention, the risk after orthopedic surgery can be as high as 60%.
-
Immobility: Long-haul travel (flights or drives longer than 8 hours), prolonged bed rest, or paralysis slows blood circulation.
-
Medical Conditions: Active cancer increases the risk 4 to 7 times. Inflammatory disorders like rheumatoid arthritis also raise the risk.
-
Hormonal Changes: Pregnancy, the postpartum period (first 6 weeks after birth), and estrogen-based medications (birth control or HRT) make the blood more likely to clot.
-
Genetics: Inherited conditions like Factor V Leiden or Antiphospholipid syndrome mean your blood naturally clots more easily.
-
Age: While it can happen at any age, the risk increases dramatically after age 55.
Symptoms of Deep Vein Thrombosis
One of the most dangerous aspects of DVT is that up to 50% of patients have no symptoms at all. When symptoms do occur, they usually only affect one leg.
Common Leg Symptoms:
-
Swelling: Often sudden and usually in just one leg.
-
Pain: Often described as a persistent cramp, soreness, or "Charlie horse" that does not go away.
-
Skin Changes: The area may feel warm to the touch and appear red or discolored (sometimes a reddish-blue).
-
Tenderness: Pain specifically when touching the leg or standing.
Emergency Symptoms (Pulmonary Embolism): If a clot has traveled to the lungs, you may experience sudden shortness of breath, sharp chest pain when breathing deeply, a rapid heart rate, or coughing up blood. Call 911 immediately if these occur.
Diagnosis of Deep Vein Thrombosis
Because symptoms can be vague or mimic other conditions like cellulitis or muscle strains, doctors use a specific sequence of tests to confirm a DVT.
-
Pretest Probability (Wells Score): Your doctor will use a checklist of your symptoms and risk factors to determine if a DVT is "likely" or "unlikely."
-
D-Dimer Test: A blood test that measures a substance released when a blood clot breaks up. If this test is normal and your risk is low, a DVT can almost always be ruled out.
-
Compression Ultrasonography: This is the primary imaging tool. It is a non-invasive ultrasound that is 95–98% accurate at finding clots in the leg by checking if the veins compress normally under pressure.
Treatment of Deep Vein Thrombosis
The main goals of treatment are to stop the clot from getting bigger, prevent it from breaking off and traveling to the lungs, and reduce the risk of future clots.
-
Anticoagulants (Blood Thinners): These are the cornerstone of treatment. They don't actually "thin" the blood or dissolve the old clot; instead, they prevent new clots from forming while your body slowly absorbs the existing one.
-
Direct Oral Anticoagulants (DOACs): Medications like Apixaban (Eliquis) or Rivaroxaban (Xarelto) are now preferred because they are convenient and do not require frequent blood monitoring.
-
Warfarin: An older option that requires regular blood tests (INR) to ensure the dosage is correct.
-
-
Duration: Most patients will need treatment for 3 to 6 months. However, if you have a recurring condition or active cancer, you may need to stay on medication indefinitely.
-
Compression Stockings: Specialized stockings (20–30 or 30–40 mmHg) help improve blood flow and can reduce the risk of Post-Thrombotic Syndrome, a long-term complication involving chronic leg pain and swelling.
-
Advanced Procedures: In severe cases, doctors may use "clot-busting" drugs (thrombolysis) or a catheter to physically remove the clot.
Prevention of Deep Vein Thrombosis
DVT is highly preventable, especially during high-risk situations like hospitalization or long-distance travel.
-
Stay Mobile: During long flights or car rides, walk around every 1–2 hours. If you can't walk, perform ankle exercises (pointing and flexing your feet) while sitting.
-
Follow Hospital Protocols: If you are having surgery, your doctor may prescribe "mini-doses" of blood thinners or use mechanical compression sleeves on your legs to keep blood moving.
-
Stay Hydrated: Drink plenty of water during travel and avoid excessive alcohol, which can lead to dehydration and thicker blood.
-
Know Your Risks: If you have a family history of clots or are planning a pregnancy, talk to your doctor about whether you should avoid estrogen-based birth control or take extra precautions during travel.




