What is Basal Cell Carcinoma?
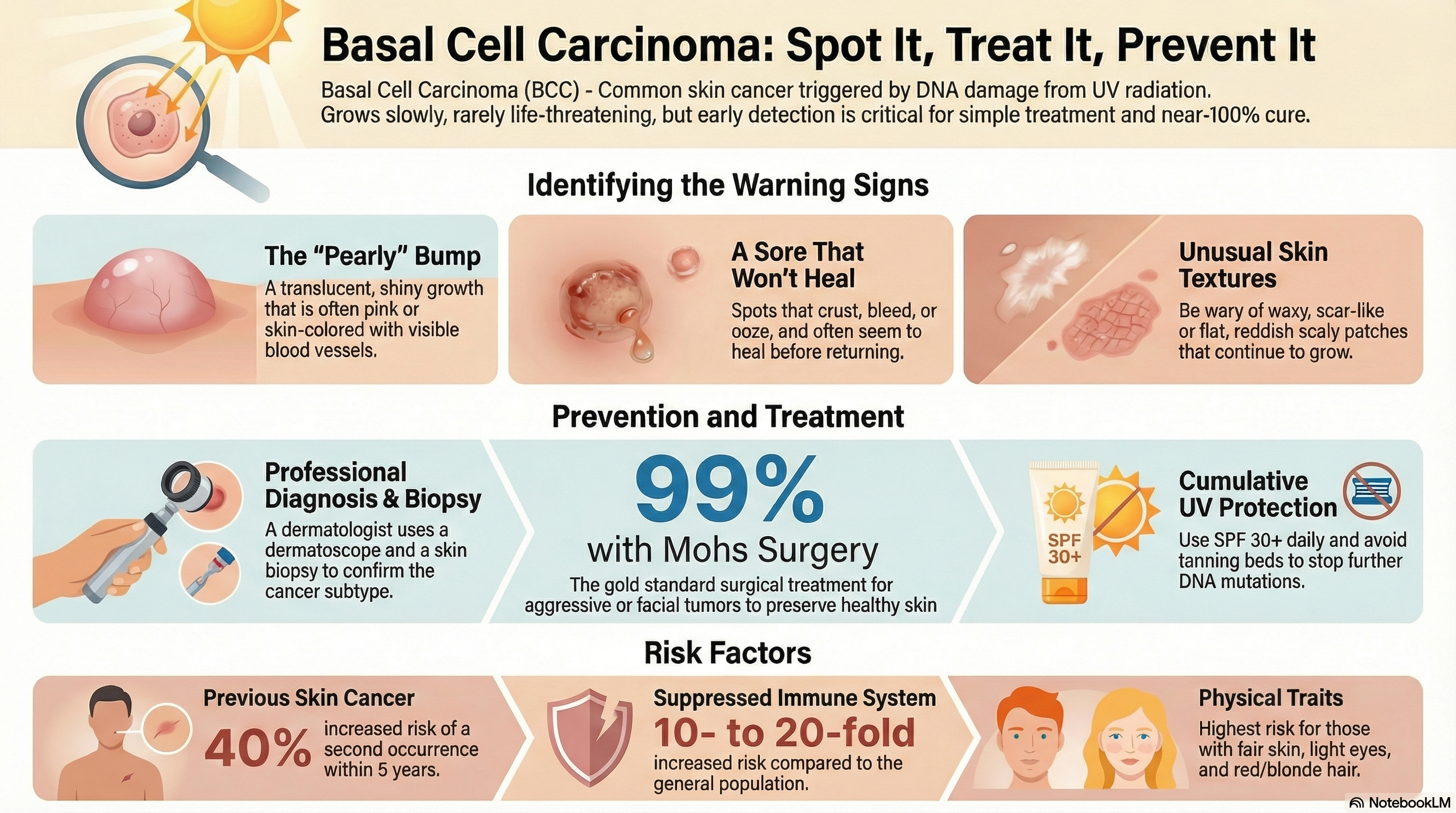
Basal cell carcinoma is a type of "keratinocyte carcinoma." It develops when DNA damage from ultraviolet (UV) radiation triggers mutations in the basal cells, leading to uncontrolled growth. It typically appears as a change in the skin, such as a growth or a sore that will not heal.
There are several different "subtypes" of BCC that look and behave differently:
-
Nodular (Most Common): A shiny, "pearly" bump that is often pink or skin-colored. You may see tiny blood vessels (telangiectasias) on the surface.
-
Superficial: A reddish, scaly patch that may look like eczema or psoriasis. These are most common on the trunk and limbs.
-
Morpheaform/Infiltrative: The most aggressive type. It often looks like a waxy, firm scar with ill-defined borders and can grow extensively beneath the surface before it is noticed.
-
Pigmented: These contain melanin and appear brown, blue, or black, sometimes mimicking a melanoma.
Causes of Basal Cell Carcinoma
The primary cause of BCC is DNA damage from ultraviolet (UV) radiation from the sun or tanning beds. This damage causes the "Hedgehog signaling pathway" in your skin cells to malfunction, telling the cells to multiply when they shouldn't.
Major Risk Factors:
-
UV Exposure: Chronic sun exposure over a lifetime or intense, intermittent exposure that leads to blistering sunburns (especially during childhood).
-
Physical Traits: Fair skin, light eyes (blue or green), and red or blonde hair. Those who always burn and never tan are at the highest risk.
-
Age and Sex: Risk increases significantly as you age, with most cases occurring after age 50. Men are diagnosed more frequently than women.
-
Medical History: A previous history of any skin cancer increases your risk of developing another by 40% within five years.
-
Immune System: People with suppressed immune systems, such as organ transplant recipients, have a 10- to 20-fold increased risk.
Symptoms of Basal Cell Carcinoma
BCC typically develops on sun-exposed areas like the face, ears, neck, scalp, shoulders, and back. Because it grows slowly, it is often painless, though it may occasionally itch or be tender.
Common signs include:
-
A Pearly Bump: A translucent, shiny growth that can be pink, white, or skin-colored.
-
A Sore That Won’t Heal: It may crust, bleed, or ooze, seemingly heal, and then return.
-
An Eczema-like Patch: A flat, scaly area of skin that continues to grow despite using moisturizers.
-
A Scar-like Area: A white, yellow, or waxy area that looks like a scar but appears where no injury occurred.
-
The "Rodent Ulcer": A nodular lesion that develops a depressed, ulcerated center with "rolled" or raised edges.
Diagnosis of Basal Cell Carcinoma
If you notice a suspicious spot, a dermatologist will perform a thorough skin examination, often using a specialized magnifying tool called a dermatoscope.
Confirmation Steps:
-
Skin Biopsy: This is the only way to confirm a diagnosis. A small sample of the growth is removed (usually via a "shave" or "punch" biopsy) and examined under a microscope.
-
Risk Stratification: Your doctor will classify the tumor as "low-risk" or "high-risk" based on its location (the nose, ears, and eyelids are high-risk "H-zones"), its size, and how aggressive the cells look under the microscope.
Treatment of Basal Cell Carcinoma
Most BCCs are easily cured if caught early. The goal of treatment is to remove the cancer completely while preserving as much healthy skin and function as possible.
Surgical Treatments (Highest Success Rates):
-
Mohs Micrographic Surgery: The gold standard for BCCs on the face or for aggressive subtypes. The surgeon removes the tumor layer by layer, checking each one under a microscope until no cancer remains. This has a 99% cure rate for new tumors.
-
Standard Surgical Excision: The tumor and a small margin of healthy skin are removed and sent to a lab.
-
Curettage and Electrodesiccation (C&E): The cancer is scraped away and the area is cauterized. This is common for small, low-risk tumors on the trunk or legs.
Non-Surgical Treatments:
-
Topical Creams: Medications like Imiquimod or 5-Fluorouracil can be used for very thin, superficial BCCs.
-
Radiation Therapy: Used for patients who cannot undergo surgery or for tumors in difficult locations.
-
Photodynamic Therapy (PDT): A light-sensitive medication is applied to the skin and then activated by a specific light source to kill cancer cells.
-
Targeted Systemic Therapy: For the extremely rare cases of advanced or metastatic BCC, oral medications (Hedgehog inhibitors like Vismodegib) can be used.
Prevention of Basal Cell Carcinoma
Since UV damage is cumulative, it is never too late to start protecting your skin.
-
Sun Protection: Seek shade, especially between 10 a.m. and 4 p.m. Wear sun-protective clothing, wide-brimmed hats, and UV-blocking sunglasses.
-
Sunscreen: Use broad-spectrum, water-resistant sunscreen with an SPF of 30 or higher every day, even when it’s cloudy.
-
Avoid Tanning Beds: There is no such thing as a "safe" tan from a tanning bed; these significantly increase your risk of all skin cancers.
-
Oral Supplements: Some studies suggest that taking Nicotinamide (a form of Vitamin B3) 500 mg twice daily can help reduce the development of new skin cancers in high-risk individuals.
-
Regular Skin Checks: Perform monthly self-exams and visit a dermatologist annually for a professional full-body skin check. Early detection makes treatment simple and nearly 100% effective.





