What is Atrial Fibrillation?
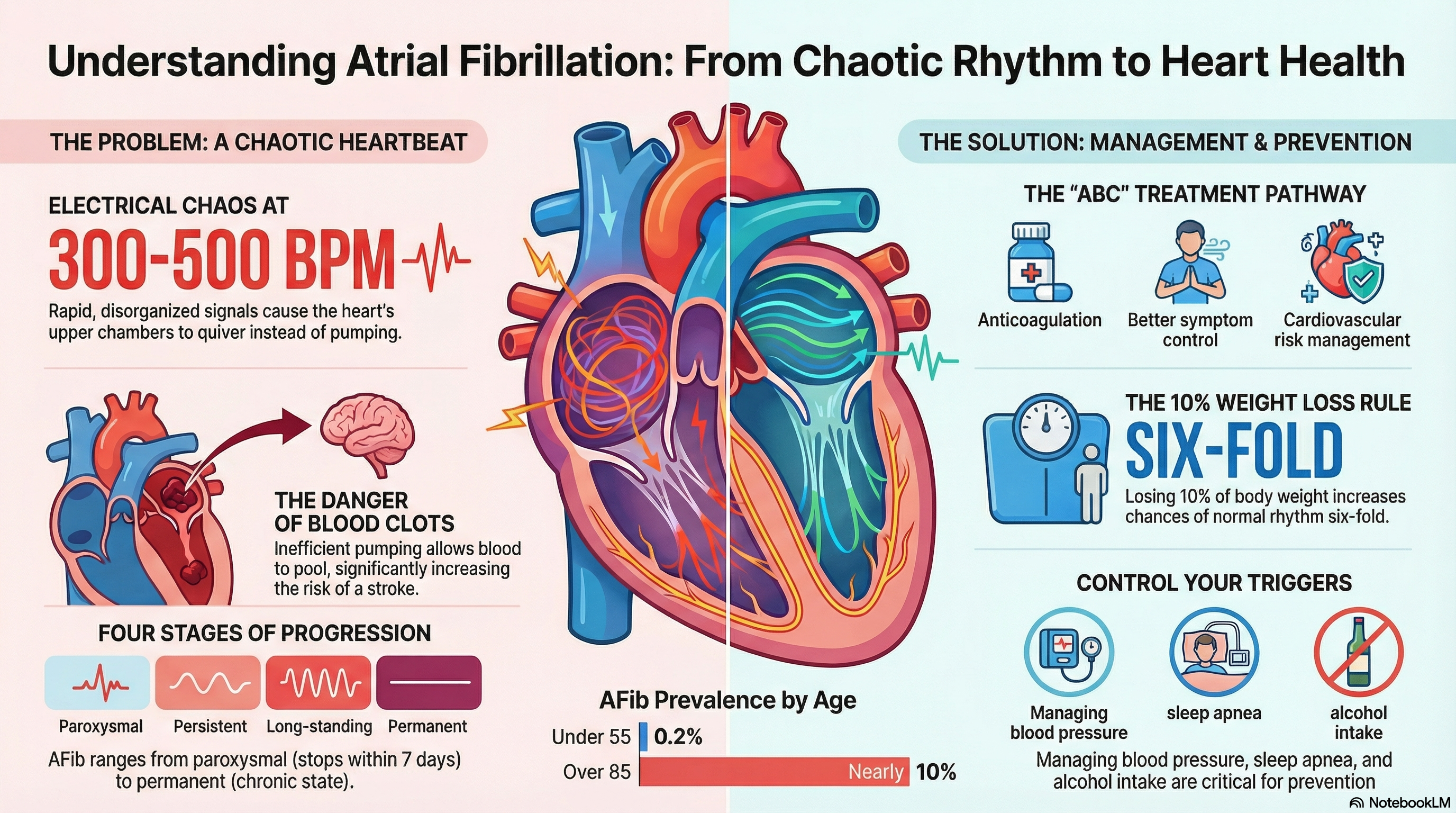
In a healthy heart, electrical signals start in the upper chambers (atria) and travel to the lower chambers (ventricles) in a steady, coordinated beat. In AFib, the electrical signals in the atria become chaotic and rapid. Instead of contracting effectively to pump blood, the atria quiver or "fibrillate" at rates of 300 to 500 beats per minute.
This chaotic activity causes the lower chambers to beat irregularly and often too fast. Because the atria aren't pumping blood efficiently, blood can pool and form clots, which may travel to the brain and cause a stroke. Doctors classify AFib into stages based on how long episodes last:
-
Paroxysmal: Episodes that start and stop on their own within 7 days.
-
Persistent: Continuous AFib that lasts more than 7 days.
-
Long-standing Persistent: Continuous AFib lasting more than 12 months.
-
Permanent: A state where the patient and doctor decide to stop trying to restore a normal rhythm.
Causes of Atrial Fibrillation
AFib can be caused by long-term damage to the heart's structure or by sudden "triggers."
Medical and Lifestyle Causes:
-
High Blood Pressure (Hypertension): The most common cause, as it puts constant stress on the heart muscle.
-
Obesity: Increased body weight can physically change the shape and electrical properties of the atria.
-
Sleep Apnea: Pauses in breathing during sleep create significant stress on the heart.
-
Heart Conditions: Previous heart attacks, coronary artery disease, and heart valve problems (especially the mitral valve).
-
Thyroid Issues: An overactive thyroid (hyperthyroidism) can "speed up" the heart's electrical system.
-
Alcohol: Even moderate drinking can trigger episodes, sometimes called "Holiday Heart Syndrome."
Non-Modifiable Factors: Age is the greatest risk factor; while only 0.2% of people under 55 have AFib, that number jumps to nearly 10% for those over 85. Family history and European ancestry also play a role in your lifetime risk.
Symptoms of Atrial Fibrillation
Up to 40% of people with AFib have no symptoms at all, and the condition is often discovered incidentally during a routine check-up or via a smartwatch. When symptoms do occur, they include:
-
Palpitations: A feeling that your heart is racing, fluttering, or skipping beats.
-
Fatigue: Feeling unusually tired or having a reduced ability to exercise.
-
Shortness of Breath: Difficulty breathing, especially during physical activity.
-
Dizziness or Lightheadedness: Feeling like you might faint (presyncope).
-
Chest Pain: Discomfort or pressure in the chest.
Diagnosis of Atrial Fibrillation
To officially diagnose AFib, a doctor must see the irregular rhythm on an electrocardiogram (ECG or EKG).
-
ECG/EKG: A 12-lead heart trace is the gold standard. It shows the absence of "P waves" (the signal of a normal atrial beat) and an irregular timing between heartbeats.
-
Ambulatory Monitoring: If your AFib comes and goes (paroxysmal), you may wear a Holter monitor, a patch, or use a smartwatch to record your heart rhythm over several days or weeks.
-
Echocardiogram: An ultrasound of the heart to check for blood clots, valve disease, or signs of heart failure.
-
Blood Tests: To check your thyroid, kidney, and liver function, as well as electrolyte levels.
Treatment of Atrial Fibrillation
Modern treatment follows the "ABC" pathway: Anticoagulation, Better symptom control, and Cardiovascular risk management.
Stroke Prevention (Anticoagulation) Doctors use the CHA₂DS₂-VASc score to determine your stroke risk. If your risk is high, you will likely be prescribed a blood thinner. Direct Oral Anticoagulants (DOACs) like apixaban or rivaroxaban are now preferred over warfarin for most patients because they have a lower risk of causing dangerous bleeding.
Symptom and Rhythm Control
-
Rate Control: Using medications like beta-blockers to keep your heart rate at a safe speed (usually under 110 beats per minute at rest).
-
Rhythm Control: Attempting to restore a normal "sinus" rhythm. This can be done with medications or a procedure called Catheter Ablation. In an ablation, a doctor uses heat or cold energy to neutralize the tiny areas of heart tissue that are triggering the chaotic signals. This is often more effective than medication for long-term relief.
Prevention of Atrial Fibrillation
While you cannot stop aging or change your genetics, lifestyle changes are incredibly powerful in preventing AFib or stopping it from getting worse.
-
Weight Management: Losing just 10% of your body weight can lead to a 6-fold increase in your chance of staying in a normal heart rhythm.
-
Blood Pressure Control: Keeping your blood pressure in a healthy range is the single most important way to protect your atria from damage.
-
Treating Sleep Apnea: Using a CPAP machine if you have sleep apnea significantly reduces AFib recurrence.
-
Moderating Alcohol: Reducing or eliminating alcohol intake helps "quiet" the heart's electrical activity.
-
Consistent Exercise: Moderate, regular activity (like brisk walking) is excellent for the heart, though extreme endurance training can sometimes increase AFib risk in certain individuals.





