What is Angina?
Angina is not a disease itself, but a critical symptom of an underlying heart problem—most commonly coronary artery disease (CAD). It is the medical term for chest pain or discomfort that occurs when your heart muscle does not receive enough oxygen-rich blood to meet its needs. This condition is known as myocardial ischemia.
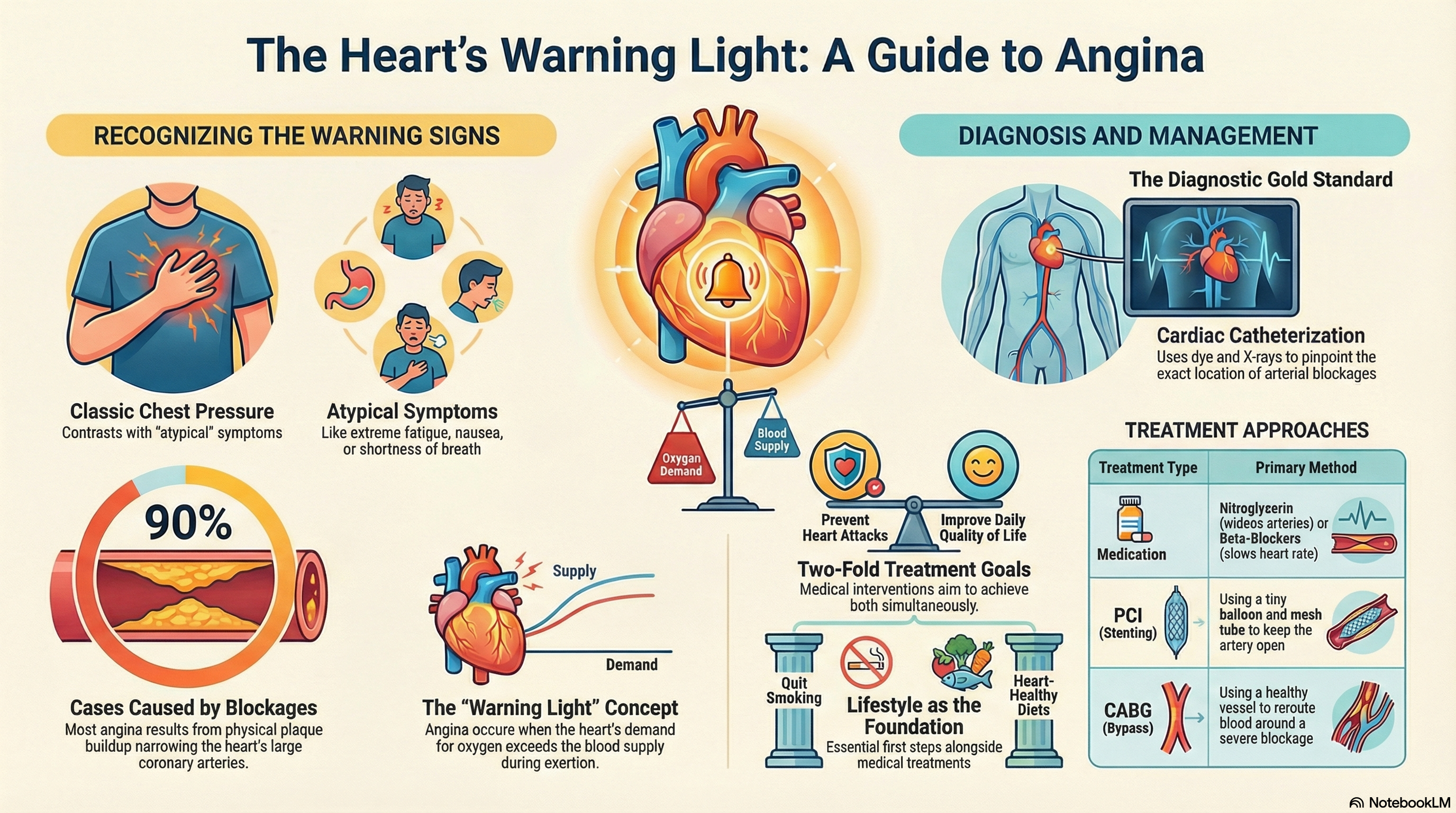
Think of angina as your heart's "warning light." When you exert yourself or experience stress, your heart works harder and requires more oxygen. If the arteries supplying the heart are narrowed by plaque, they cannot deliver that extra blood, leading to the sensation of angina. While it can be frightening, identifying and treating angina early can prevent more serious events like a heart attack.
Causes of Angina
The most frequent cause of angina is the narrowing of the coronary arteries due to a buildup of fatty deposits called plaque (atherosclerosis). However, there are several ways this reduced blood flow can occur, which defines the type of angina you may have:
Obstructive Coronary Artery Disease In more than 90% of cases, physical blockages in the large arteries of the heart restrict blood flow. This is the primary cause of Stable Angina, which follows a predictable pattern during physical exertion.
Coronary Artery Spasm This causes Variant (Prinzmetal's) Angina. The arteries are not necessarily blocked by plaque, but they suddenly "spasm" or tighten, often at rest during the early morning hours.
Microvascular Dysfunction This causes Microvascular Angina, where the smallest blood vessels of the heart do not function correctly. This is more commonly seen in women and can occur even if the large arteries look clear.
Risk Factors Several factors increase your likelihood of developing the arterial damage that leads to angina, including:
-
Smoking and tobacco use
-
High blood pressure and high cholesterol
-
Diabetes and obesity
-
A sedentary lifestyle and chronic stress
-
Family history of heart disease
Symptoms of Angina
Angina is most famously described as chest pain, but the sensation can vary significantly between individuals.
Classic Symptoms Typical angina is described as a feeling of squeezing, tightness, pressure, or heaviness in the center of the chest. This discomfort may radiate to:
-
The left arm (most common) or both arms
-
The neck and jaw
-
The shoulders or back
-
The upper stomach (epigastric area)
Anginal Equivalents (Atypical Symptoms) Some people, particularly women, the elderly, and those with diabetes, may not feel chest pressure at all. Instead, they experience "anginal equivalents," which include:
-
Shortness of breath (dyspnea)
-
Extreme or unusual fatigue
-
Nausea or indigestion-like burning
-
Sweating and dizziness
Diagnosis of Angina
A doctor begins the diagnostic process with a detailed history of your symptoms and a physical exam. Because stable angina often does not show up on a resting EKG, specialized tests are required to see how the heart performs under stress.
Stress Testing You may be asked to walk on a treadmill or receive a medication that mimics exercise while your heart's electrical activity (EKG) or blood flow (Nuclear Stress Test) is monitored.
Imaging Tests
-
Coronary CT Angiography (CCTA): A specialized CT scan that provides a high-resolution 3D map of your heart's arteries to identify blockages.
-
Echocardiogram: An ultrasound of the heart to see how the muscle walls and valves are moving.
Cardiac Catheterization Considered the "gold standard" for diagnosis, a thin tube is guided to the heart, and dye is injected to show the exact location and severity of blockages under X-ray.
Treatment of Angina
The goals of treatment are twofold: to prevent major cardiovascular events (like heart attacks) and to improve your quality of life by reducing symptoms.
Lifestyle Modifications This is the foundation of treatment. It includes quitting smoking, losing weight, and adopting a heart-healthy diet, such as the Mediterranean diet. Regular, supervised exercise is also critical for improving your heart's efficiency.
Medications
-
Nitroglycerin: Taken as a spray or small pill under the tongue to quickly widen arteries and stop an active attack.
-
Beta-Blockers: These are the first-line treatment to slow the heart rate and reduce the heart's demand for oxygen.
-
Statins: High-dose statins are used to stabilize plaque and lower cholesterol levels.
-
Anti-clotting agents: Aspirin is commonly prescribed to prevent blood clots from forming in narrowed arteries.
Medical Procedures If medications are not enough, a doctor may recommend:
-
PCI (Stenting): Using a tiny balloon to open the artery and a mesh tube (stent) to keep it open.
-
CABG (Bypass Surgery): Using a healthy vessel from another part of your body to "bypass" a severely blocked artery.
Prevention of Angina
While some risk factors like age and family history cannot be changed, the majority of angina triggers are preventable through proactive heart care.
Aggressive Risk Control Managing chronic conditions is the most effective prevention strategy. If you have diabetes or high blood pressure, keeping these within a healthy range significantly slows the progression of artery damage.
Healthy Habits
-
Diet: Focus on vegetables, fruits, whole grains, and healthy fats.
-
Activity: Aim for at least 30 to 45 minutes of moderate exercise most days of the week.
-
Avoidance: Stay away from secondhand smoke and manage emotional stress through mindfulness or counseling.
When to Seek Emergency Help You should call emergency services immediately if your chest pain occurs at rest, lasts longer than 15 minutes, or is not relieved by three doses of nitroglycerin. This may indicate Unstable Angina, which is a medical emergency and a precursor to a heart attack.





