What is Anaphylaxis?
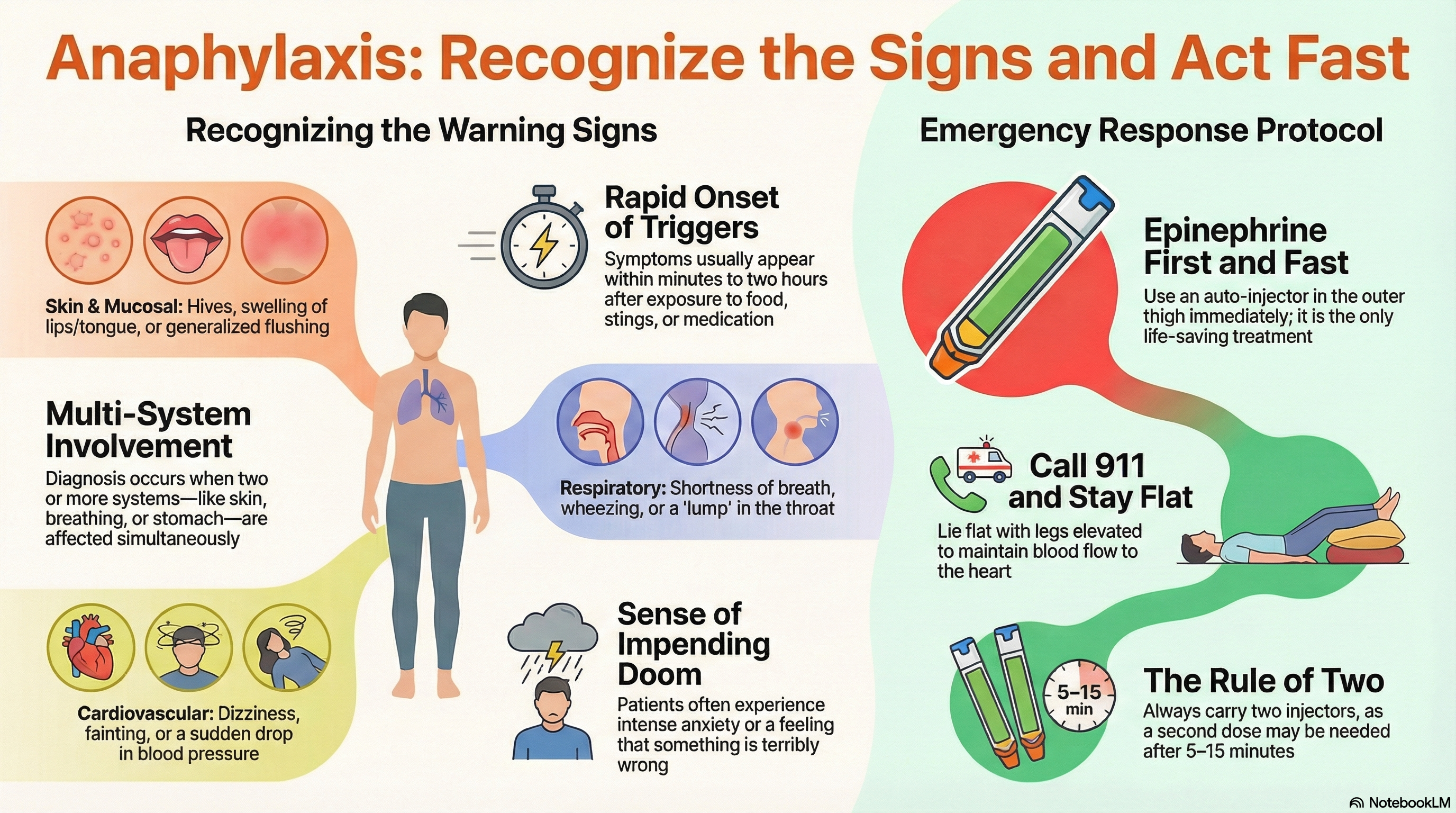
Anaphylaxis is a severe, life-threatening allergic reaction that affects the entire body. It is characterized by a rapid onset—usually within minutes to two hours after exposure to a trigger—and involves multiple organ systems at once.
When you encounter an allergen, your immune system overreacts by releasing a massive flood of chemicals, such as histamine and tryptase. This "mediator release" causes your blood vessels to leak fluid (leading to swelling and a drop in blood pressure) and your airways to constrict. Because it can quickly lead to airway obstruction and shock, anaphylaxis is always a medical emergency.
Causes of Anaphylaxis
Almost any substance can trigger anaphylaxis, but most cases are caused by a few common categories of allergens.
Common Triggers:
-
Foods: The leading cause in children and young adults. Common culprits include peanuts, tree nuts (walnuts, cashews), shellfish, fish, milk, eggs, soy, wheat, and sesame.
-
Insect Stings: Venoms from bees, wasps, hornets, yellow jackets, and fire ants.
-
Medications: Antibiotics (like penicillin), aspirin, ibuprofen (NSAIDs), and certain anesthesia or chemotherapy drugs.
-
Latex: Found in medical gloves, balloons, and some dental products.
-
Exercise: In rare cases, physical activity can trigger a reaction, sometimes only if a specific food was eaten shortly before the workout.
-
Idiopathic: In up to 20% of cases, a specific trigger cannot be identified even after professional testing.
Symptoms of Anaphylaxis
Symptoms of anaphylaxis are "systemic," meaning they impact various parts of the body simultaneously. A diagnosis is typically made when two or more of the following systems are involved.
Skin and Mucosal (Most Common)
-
Itchy, raised red welts (hives) or generalized flushing.
-
Significant swelling (angioedema) of the lips, tongue, face, or around the eyes.
Respiratory (Most Dangerous)
-
Shortness of breath, wheezing, or a persistent cough.
-
A hoarse voice or trouble swallowing.
-
A feeling that the throat is closing or a "lump" in the throat.
Cardiovascular and Neurological
-
Hypotension: A sudden, dangerous drop in blood pressure.
-
Dizziness, lightheadedness, or fainting.
-
A weak, rapid pulse.
-
A "sense of impending doom" or severe anxiety.
Gastrointestinal
-
Severe abdominal cramps or pain.
-
Nausea, vomiting, or diarrhea.
Diagnosis of Anaphylaxis
Anaphylaxis is a clinical diagnosis, meaning it is identified by a doctor based on your symptoms and the timing of the reaction. Treatment must never be delayed for testing.
Diagnostic Criteria: Doctors look for the rapid onset of skin or mucosal symptoms combined with either respiratory distress or a drop in blood pressure. In some cases, such as an insect sting, a sudden drop in blood pressure alone is enough to confirm the diagnosis.
Follow-up Testing:
-
Tryptase Test: A blood test taken within 1 to 4 hours of the reaction can confirm that a massive immune cell release occurred.
-
Allergy Testing: Once the emergency has passed, an allergist will use skin prick tests or blood tests to identify the specific trigger to help you avoid it in the future.
Treatment of Anaphylaxis
Immediate action is the most important factor in surviving anaphylaxis.
1. Epinephrine (Adrenaline) First Epinephrine is the only life-saving treatment for anaphylaxis. It quickly reverses the reaction by opening the airways and raising blood pressure.
-
Use an auto-injector (like an EpiPen® or Auvi-Q®) immediately in the outer thigh.
-
It can be injected through clothing.
-
If symptoms don't improve in 5–15 minutes, a second dose should be administered.
2. Call Emergency Services Even if you feel better after the injection, you must go to the hospital. You may experience a biphasic reaction, which is a second wave of symptoms that can occur up to 12 hours later without being re-exposed to the trigger.
3. Proper Positioning
-
Lie flat on your back with your legs elevated to help blood reach your heart.
-
If you are vomiting or struggling to breathe, sit up or lie on your side, but do not stand or walk, as this can cause a fatal drop in blood pressure.
Secondary Treatments: Once at the hospital, doctors may provide oxygen, IV fluids, and secondary medications like antihistamines or steroids. Note that these cannot stop a life-threatening reaction on their own; they are only used after epinephrine.
Prevention of Anaphylaxis
Prevention focuses on strict avoidance of known triggers and being prepared for an accidental exposure.
Stay Prepared:
-
Carry Two Auto-Injectors: Always have two epinephrine injectors with you. One dose is not always enough to stop a severe reaction.
-
Emergency Action Plan: Work with your doctor to create a written plan that tells others (teachers, coworkers, friends) exactly how to recognize your symptoms and use your injector.
-
Medical Alert Jewelry: A bracelet or necklace can speak for you if you become unconscious or unable to talk.
Risk Reduction:
-
Allergen Avoidance: Carefully read food labels and inform restaurant staff of your allergies.
-
Manage Underlying Health: Conditions like asthma, especially if poorly controlled, increase the risk of a fatal reaction.
-
Allergist Referral: Regular follow-ups with an allergist can help you stay informed about new treatments and ensure your action plan is up to date.





