What is Amyloidosis?
Amyloidosis is a rare but serious group of diseases caused by the buildup of abnormal proteins in the body's organs and tissues. These proteins, which have "misfolded" into an irregular shape, clump together to form insoluble deposits called amyloid fibrils.
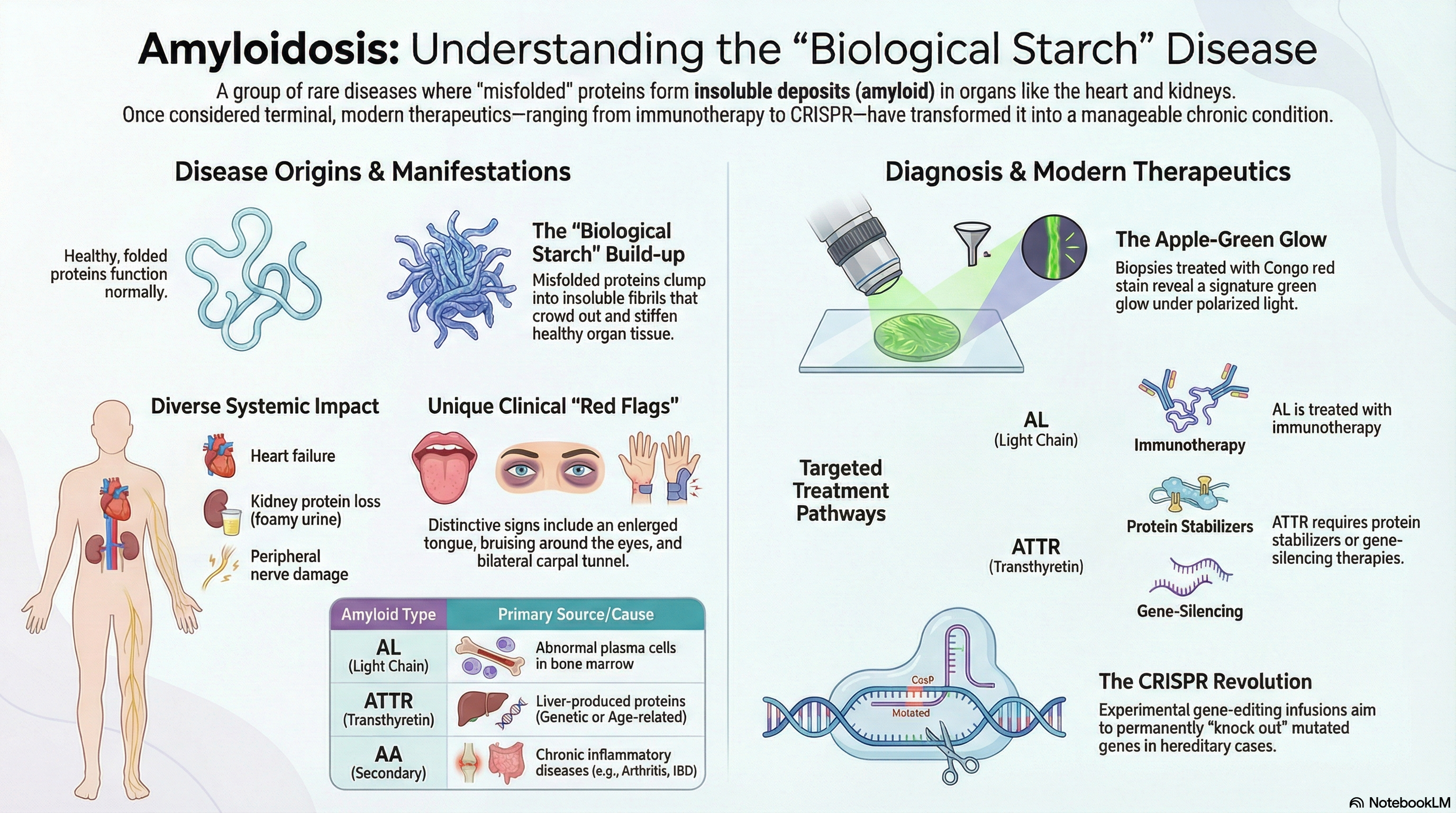
Think of amyloid as a type of biological "starch" that the body cannot easily break down. As these deposits grow, they crowd out healthy tissue, causing organs to become stiff and eventually fail. Amyloidosis is not a single disease; it is categorized based on the specific type of protein that is misfolding. While it can affect almost any part of the body, it most commonly impacts the heart, kidneys, liver, and nervous system.
Causes of Amyloidosis
The cause of amyloidosis depends entirely on the type of protein involved. There are over 40 different proteins that can form amyloid, but three types are most common:
AL Amyloidosis (Light Chain): This is the most common systemic form. It is caused by abnormal plasma cells in the bone marrow (similar to the cells involved in multiple myeloma). These cells produce misfolded "light chain" proteins that enter the bloodstream and deposit in organs.
ATTR Amyloidosis (Transthyretin): This involves a protein called transthyretin, which is produced in the liver. It comes in two forms:
-
Hereditary (ATTRv): Caused by a genetic mutation passed down through families. One specific mutation (Val122Ile) is found in about 3.4% of the U.S. Black population.
-
Wild-Type (ATTRwt): An age-related condition, usually affecting men over 70, where the normal protein begins to misfold over time.
AA Amyloidosis (Secondary): This results from chronic inflammatory diseases (like rheumatoid arthritis or IBD). Constant inflammation causes the body to overproduce "Serum Amyloid A" protein, which eventually deposits in the organs, particularly the kidneys.
Symptoms of Amyloidosis
Because amyloidosis can affect many different organs, symptoms are often vague and can mimic more common conditions. Early signs often include unexplained fatigue, weight loss, and shortness of breath.
Organ-Specific Symptoms:
-
Heart: Shortness of breath, swelling in the legs (edema), and palpitations. This is often "heart failure with preserved ejection fraction."
-
Kidneys: Foamy urine (a sign of protein loss) and severe leg swelling.
-
Nervous System: Numbness, tingling, or "pins and needles" in the hands and feet (peripheral neuropathy), or dizziness when standing up (orthostatic hypotension).
-
Soft Tissue: Distinctive signs include an enlarged tongue (macroglossia), carpal tunnel syndrome in both wrists, and "raccoon eyes" (bruising around the eyes).
Diagnosis of Amyloidosis
Early and accurate diagnosis is critical because the treatments for different types of amyloidosis are completely different.
Biopsy and Staining The "gold standard" for diagnosis is a tissue biopsy (often from an abdominal fat pad or the affected organ). This tissue is treated with Congo red stain. Under a special polarized light, amyloid deposits show a characteristic "apple-green" glow, confirming the diagnosis.
Typing the Protein Once amyloid is found, it must be typed. This is usually done through mass spectrometry to ensure the patient receives the correct treatment (e.g., treating AL amyloidosis with ATTR drugs will not work).
Non-Invasive Testing For heart-related ATTR amyloidosis, doctors can now use a specialized "bone tracer" scan (technetium-based scintigraphy). If the scan shows the heart "lighting up" and blood tests rule out light chain issues, a diagnosis can be made without a heart biopsy.
Treatment of Amyloidosis
In the last few years, treatment for amyloidosis has been revolutionized, turning what was once a terminal diagnosis into a manageable chronic condition for many.
Treating AL Amyloidosis The goal is to stop the production of the abnormal protein by targeting the plasma cells.
-
Chemotherapy and Immunotherapy: Regimens including the monoclonal antibody daratumumab have significantly improved survival rates.
-
Stem Cell Transplant: In eligible patients, a high-dose chemotherapy treatment followed by a transplant can lead to long-term remission.
Treating ATTR Amyloidosis
-
Stabilizers: Medications like tafamidis act like "glue" to keep the transthyretin protein from falling apart and misfolding.
-
Gene Silencers: Newer therapies (like patisiran and vutrisiran) work by "turning off" the production of the protein in the liver.
-
CRISPR Technology: As of 2025–2026, experimental gene-editing treatments are showing promise in permanently "knocking out" the mutated gene with a single infusion.
Prevention of Amyloidosis
Because most forms of amyloidosis are either caused by spontaneous cell mutations, genetics, or aging, there is no guaranteed way to prevent the disease. However, risk management is possible.
Managing Inflammation For AA Amyloidosis, the best prevention is the aggressive treatment of underlying inflammatory conditions like arthritis or chronic infections. Modern management of these diseases has made AA amyloidosis much rarer today.
Genetic Screening If you have a family history of hereditary (ATTRv) amyloidosis, genetic counseling and screening can help identify the risk before symptoms appear. This allows for early monitoring and the start of "gene silencer" therapies at the first sign of disease.
Awareness and Early Detection The most effective way to prevent severe organ damage is early detection. If you have "red flag" symptoms like bilateral carpal tunnel syndrome combined with heart failure or protein in the urine, ask your doctor about amyloidosis. Early treatment can halt the deposition of new amyloid and protect your organ function.





